July 2024
Symptoms and Risk Factors for Toenail Fungus
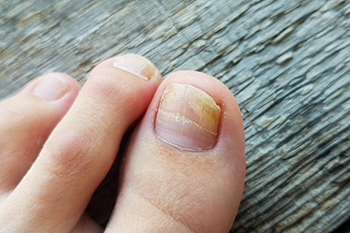
Toenail fungus, also known as onychomycosis, is a fungal infection affecting the toenails. It typically begins as a white or yellow spot under the tip of the nail and can spread deeper into the nail over time, causing discoloration, thickening, and crumbling of the nail edges. Risk factors for toenail fungus include frequent exposure to warm and moist environments such as public showers, wearing tight-fitting shoes, and having a weakened immune system. Symptoms may include a foul odor from the infected nail, pain or discomfort, and difficulty trimming the nail due to its thickness. If left untreated, toenail fungus can lead to permanent damage to the nail bed and spread to other nails or skin. The chances of recovery increase when treated early. If you have toenail fungus, it is suggested that you contact a podiatrist where you can receive expert treatment for this condition.
For more information about treatment, contact John Killough, DPM of Regional Foot Center. Our doctor can provide the care you need to keep you pain-free and on your feet.
Toenail Fungus Treatment
Toenail fungus is a condition that affects many people and can be especially hard to get rid of. Fortunately, there are several methods to go about treating and avoiding it.
Antifungals & Deterrence
Oral antifungal medicine has been shown to be effective in many cases. It is important to consult with a podiatrist to determine the proper regiment for you, or potentially explore other options.
Applying foot powder on the feet and shoes helps keep the feet free of moisture and sweat.
Sandals or open toed shoes – Wearing these will allow air movement and help keep feet dry. They also expose your feet to light, which fungus cannot tolerate. Socks with moisture wicking material also help as well.
If you have any questions please feel free to contact our offices located in Charleston and Effingham, IL . We offer the newest diagnostic tools and technology to treat your foot and ankle needs.
How to Identify and Treat a Foot Corn
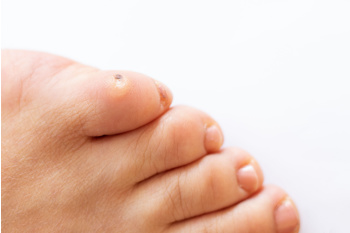
Corns, those pesky patches of thickened skin, can turn a simple walk into agony. Identifying them is key. Look for hardened areas on toes or feet, often with a cone-like shape pointing inward. They are caused by friction and pressure, typically from wearing ill-fitting shoes or repetitive actions. Treating corns involves gentle methods like soaking the feet in warm water, using a pumice stone to smooth the area, and moisturizing to prevent recurrence. Avoid over-the-counter corn removal products, as they can damage healthy skin. For persistent corns, or if you are unsure about treatment, it is wise to seek advice from a podiatrist. They can provide professional care, assess your foot health, and recommend appropriate courses of action. Do not let corns slow you down. It is suggested that you schedule an appointment with a podiatrist for personalized guidance and relief.
If you have any concerns regarding your feet and ankles, contact John Killough, DPM of Regional Foot Center. Our doctor will treat your foot and ankle needs.
Corns: What Are They? and How Do You Get Rid of Them?
Corns can be described as areas of the skin that have thickened to the point of becoming painful or irritating. They are often layers and layers of the skin that have become dry and rough, and are normally smaller than calluses.
Ways to Prevent Corns
There are many ways to get rid of painful corns such as wearing:
- Well-fitting socks
- Comfortable shoes that are not tight around your foot
- Shoes that offer support
Treating Corns
Treatment of corns involves removing the dead skin that has built up in the specific area of the foot. Consult with Our doctor to determine the best treatment option for your case of corns.
If you have any questions please feel free to contact our offices located in Charleston and Effingham, IL . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Debridement Methods for Diabetic Foot Ulcers
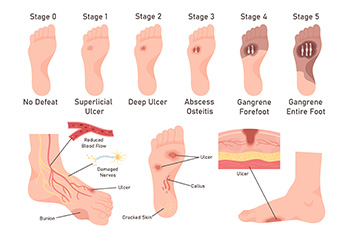
Debridement is a key procedure in managing diabetic foot ulcers, involving a podiatrist removing dead and infected tissue to promote healing and prevent infection spread. This process is vital because the buildup of necrotic tissue can obscure the true extent of the ulcer. There are several methods of debridement. Surgical debridement involves a podiatrist using tools like scalpels to precisely remove dead tissue, often performed at the bedside or in an operating room for more severe cases. Mechanical debridement employs saline-soaked pads that adhere to and remove dead tissue upon removal, though this can be painful and may also disturb healthy tissue. Chemical debridement uses enzymes to dissolve dead material. Biological debridement, utilizing maggots, effectively cleanses wounds by consuming only dead tissue. Before any debridement, the podiatrist will assess the patient’s overall health, and the wound will be cleaned with a saline solution. If you have diabetic foot ulcers, it is suggested that you make a podiatrist a part of your medical team for expert wound care options.
Wound care is an important part in dealing with diabetes. If you have diabetes and a foot wound or would like more information about wound care for diabetics, consult with John Killough, DPM from Regional Foot Center. Our doctor will assess your condition and provide you with quality foot and ankle treatment.
What Is Wound Care?
Wound care is the practice of taking proper care of a wound. This can range from the smallest to the largest of wounds. While everyone can benefit from proper wound care, it is much more important for diabetics. Diabetics often suffer from poor blood circulation which causes wounds to heal much slower than they would in a non-diabetic.
What Is the Importance of Wound Care?
While it may not seem apparent with small ulcers on the foot, for diabetics, any size ulcer can become infected. Diabetics often also suffer from neuropathy, or nerve loss. This means they might not even feel when they have an ulcer on their foot. If the wound becomes severely infected, amputation may be necessary. Therefore, it is of the upmost importance to properly care for any and all foot wounds.
How to Care for Wounds
The best way to care for foot wounds is to prevent them. For diabetics, this means daily inspections of the feet for any signs of abnormalities or ulcers. It is also recommended to see a podiatrist several times a year for a foot inspection. If you do have an ulcer, run the wound under water to clear dirt from the wound; then apply antibiotic ointment to the wound and cover with a bandage. Bandages should be changed daily and keeping pressure off the wound is smart. It is advised to see a podiatrist, who can keep an eye on it.
If you have any questions, please feel free to contact our offices located in Charleston and Effingham, IL . We offer the newest diagnostic and treatment technologies for all your foot care needs.
What to Do About Heel Pain
 Heel pain, often linked to conditions such as plantar fasciitis, is a prevalent complaint that affects the bottom or back of the heel. This pain typically results from inflammation, overuse, or injury to the plantar fascia, a thick band of tissue that supports the arch of the foot. Factors contributing to heel pain include excessive walking or standing, wearing improper footwear, obesity, and age-related changes. The pain is usually sharp and most intense during the first steps in the morning or after long periods of rest. It can significantly interfere with daily activities, making walking, exercising, and even standing difficult. Diagnosis involves a physical examination, patient history, and sometimes imaging tests like X-rays or MRI scans to rule out fractures or other issues. Treatment typically includes rest, anti-inflammatory medications, and stretching exercises. Custom orthotics and targeted stretching exercises may also be recommended. If you have persistent or severe heel pain, it is suggested that you schedule an appointment with a podiatrist for specialized care and treatment.
Heel pain, often linked to conditions such as plantar fasciitis, is a prevalent complaint that affects the bottom or back of the heel. This pain typically results from inflammation, overuse, or injury to the plantar fascia, a thick band of tissue that supports the arch of the foot. Factors contributing to heel pain include excessive walking or standing, wearing improper footwear, obesity, and age-related changes. The pain is usually sharp and most intense during the first steps in the morning or after long periods of rest. It can significantly interfere with daily activities, making walking, exercising, and even standing difficult. Diagnosis involves a physical examination, patient history, and sometimes imaging tests like X-rays or MRI scans to rule out fractures or other issues. Treatment typically includes rest, anti-inflammatory medications, and stretching exercises. Custom orthotics and targeted stretching exercises may also be recommended. If you have persistent or severe heel pain, it is suggested that you schedule an appointment with a podiatrist for specialized care and treatment.
Many people suffer from bouts of heel pain. For more information, contact John Killough, DPM of Regional Foot Center. Our doctor can provide the care you need to keep you pain-free and on your feet.
Causes of Heel Pain
Heel pain is often associated with plantar fasciitis. The plantar fascia is a band of tissues that extends along the bottom of the foot. A rip or tear in this ligament can cause inflammation of the tissue.
Achilles tendonitis is another cause of heel pain. Inflammation of the Achilles tendon will cause pain from fractures and muscle tearing. Lack of flexibility is also another symptom.
Heel spurs are another cause of pain. When the tissues of the plantar fascia undergo a great deal of stress, it can lead to ligament separation from the heel bone, causing heel spurs.
Why Might Heel Pain Occur?
- Wearing ill-fitting shoes
- Wearing non-supportive shoes
- Weight change
- Excessive running
Treatments
Heel pain should be treated as soon as possible for immediate results. Keeping your feet in a stress-free environment will help. If you suffer from Achilles tendonitis or plantar fasciitis, applying ice will reduce the swelling. Stretching before an exercise like running will help the muscles. Using all these tips will help make heel pain a condition of the past.
If you have any questions please contact our offices located in Charleston and Effingham, IL . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Gout Pain Can Be Managed
Risk of Foot Stress Fractures in Runners

The popularity of running for fitness and exercise has led to a rise in stress fractures of the foot. These injuries are often seen in first-time runners who enter races with inadequate or improper training. The repetitive impact of running can cause hairline fractures in the foot bones, especially when mileage is increased too quickly or training becomes more intense without sufficient rest. Runners at all levels risk stress fractures if they wear unsuitable shoes, have flat feet or bunions, or osteoporosis. Symptoms of a stress fracture include pain, swelling, redness, and bruising. Pain often subsides after activity. Early diagnosis and treatment are vital for proper healing to prevent the fracture from progressing to a complete break. Runners can reduce their risk of stress fractures by wearing supportive athletic shoes and gradually increasing their activity levels. If you are experiencing foot pain after running, it is suggested that you schedule an appointment with a podiatrist for an exam and treatment.
Activities where too much pressure is put on the feet can cause stress fractures. To learn more, contact John Killough, DPM from Regional Foot Center. Our doctor can provide the care you need to keep your pain free and on your feet.
Dealing with Stress Fractures of the Foot and Ankle
Stress fractures occur in the foot and ankle when muscles in these areas weaken from too much or too little use. The feet and ankles then lose support when walking or running from the impact of the ground. Since there is no protection, the bones receive the full impact of each step. Stress on the feet can cause cracks to form in the bones, thus creating stress fractures.
What Are Stress Fractures?
Stress fractures occur frequently in individuals whose daily activities cause great impact on the feet and ankles. Stress factors are most common among:
- Runners
- People affected with Osteoporosis
- Tennis or basketball players
- Gymnasts
- High impact workouts
Symptoms
Pain from the fractures occur in the area of the fractures and can be constant or intermittent. It will often cause sharp or dull pain with swelling and tenderness. Engaging in any kind of activity which involves high impact will aggravate pain.
If you have any questions please feel free to contact our offices located in Charleston and Effingham, IL . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.





